The thoracic form of osteochondrosis is characterized by degenerative damage to the intervertebral cartilage and secondary changes in the thoracic vertebrae. Diagnosis of the disease is sometimes quite problematic, since it is often "masked" as other pathologies: myocardial infarction, angina, pathologies of the gastrointestinal tract.
Features of thoracic osteochondrosis.
This type of disease is quite rare compared to cervical and lumbar.
The reason lies in the peculiarities of the anatomical structure of the thoracic region:
- it is the longest (it consists of 12 vertebrae);
- in this area there is a slight natural curvature: the physiological kyphosis, which relieves part of the load resulting from walking upright;
- the thoracic region is articulated with the ribs and the sternum, which perform the functions of a physiological frame and take on the main load;
- in cross section, the spinal canal of the thoracic region has the smallest dimensions;
- The thoracic vertebrae are thinner and smaller, but have long spinous processes.
As a result of these factors, the thoracic part is not particularly mobile, so osteochondrosis in this part of the spine is rare, but its symptoms are quite pronounced: they are quite strong and unpleasant pains associated with pinching of the spinal nerves, that irritate the shoulder. waist and upper limbs organs located in the abdominal cavity and thorax. For the same reasons, the manifestations of the thoracic form of osteochondrosis are usually atypical, which significantly complicates the diagnosis of pathology and subsequent treatment.
The narrowness of the spinal canal, the presence of physiological kyphosis and the relatively small size of the vertebrae create the most favorable conditions for the formation of intervertebral disc herniations. Since a significant part of the load falls mainly on the anterior and lateral parts of the vertebral bodies and discs, the disc shifts posteriorly and a herniated disc or Schmorl's herniation is formed.
The anterior part of the vertebrae is subject to greater stress than the posterior part. For this reason, very often the growth of osteophytes and prolapse of intervertebral discs occurs outside the spinal column and does not affect the spinal cord.
Stages of thoracic osteochondrosis.
The manifestations of thoracic osteochondrosis are determined by the changes that occur in the discs and vertebrae, according to which four main stages of the disease are distinguished:
- Stage I is characterized by dehydration of the intervertebral discs, as a result of which they lose elasticity and firmness, but still retain the ability to withstand normal loads. The process of flattening the disc begins, its height reduces and bulges form. The pain at this stage is mild.
- In stage II, cracks form in the annulus fibrosus and instability of the entire segment is recorded. Painful sensations become more intense and intensify when bending and with some other movements.
- A characteristic sign of stage III is the rupture of the annulus fibrosus and the beginning of the formation of a herniated intervertebral disc.
- During the transition to stage IV, due to the lack of disc resistance, the vertebrae begin to move closer together, which causes spondyloarthrosis (disorders in the intervertebral joints) and spondylolisthesis (torsion or displacement of the vertebrae). The mobilization of compensatory forces to reduce the load leads to growth of the vertebra, an increase in its area and its flattening. The affected part of the annulus fibrosus begins to be replaced by bone tissue, which significantly limits the motor capabilities of the section.
Degrees of thoracic osteochondrosis.
Today, many specialists use a different classification principle, according to which the course of osteochondrosis of the thoracic spine is distinguished not by stages, but by degrees with their characteristic features.
How does first degree disease manifest? As a general rule, it is diagnosed when an intervertebral disc ruptures, caused by excessive effort or sudden movement. In this case, sharp pain suddenly occurs in the spine. Patients compare it to the passage of electrical current through the spine. This condition is accompanied by reflex tension of all muscles.
We speak of second degree of thoracic osteochondrosis in cases where instability of the spine appears and symptoms of protrusion of the intervertebral discs develop. This condition is very rare, occurs with periods of exacerbation and subsequent remission, and is detected only with a thorough diagnostic examination.
What symptoms appear in third degree disease? The pain becomes constant, radiates along the damaged nerve and is accompanied by partial loss of sensation in the upper or lower extremities, changes in gait and severe headaches. At this stage, shortness of breath and disruption of the normal heart rhythm are often observed.
We can talk about moving to the fourth degree when the manifestations of the disease decrease while the symptoms of spinal instability persist (sliding, twisting of the vertebrae, fixation with each other). Osteophytes begin to grow, gradually pinching the spinal nerves and compressing the spinal cord.
Typical symptoms and signs.
Osteochondrosis of the thoracic region has quite characteristic signs, according to which this disease is most likely to be diagnosed:
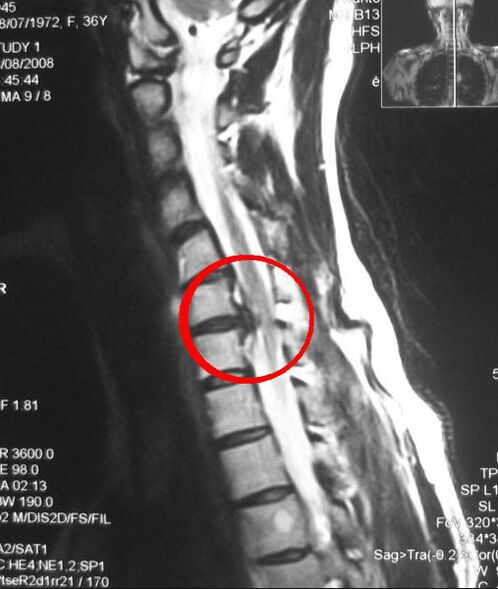
- Intercostal neuralgia - often the pain is localized in one area, after which it quickly spreads to the entire chest, forcing patients to be in a certain position and significantly complicating breathing.
- When turning, neck movements, bending, raising arms, respiratory acts (inhalation-exhalation), the pain becomes much more intense.
- The muscles of the middle and upper back go into severe spasm. It is also possible to contract the muscle fibers of the abdominals, lower back and shoulder girdle, which is reflex in nature (develops as a reaction to acute pain syndrome).
- Intercostal neuralgia is usually preceded by pain, stiffness, and a feeling of discomfort that occurs in the chest and back when moving. The pain can be quite intense and last for several weeks without spreading further, after which it gradually begins to disappear.
- All symptoms become more pronounced at night. In the morning they significantly soften or decrease, intensifying with hypothermia, movements (especially vibratory and sudden), and may manifest themselves in the form of a certain rigidity.
Atypical symptoms and signs.
Often, the symptoms of osteochondrosis located in the chest area resemble those of other diseases.
- Imitation of the pain characteristic of cardiac pathologies (heart attack, angina). This pain can be quite long-lasting (unlike cardialgia), while traditional drugs used to dilate the coronary vessels do not eliminate the pain. The cardiogram also shows no changes.
- In the acute stage of thoracic osteochondrosis, prolonged (up to several weeks) pain in the sternum often occurs, reminiscent of diseases of the mammary glands. They can be excluded by examination by a mammologist.
- Pain in the abdomen (iliac region) resembles colitis or gastritis. When located in the right upper quadrant, cholecystitis, pancreatitis or hepatitis are often misdiagnosed. These symptoms are usually accompanied by alterations in the digestive system due to damage to its innervation. In such cases, it is necessary to identify thoracic osteochondrosis as the main disease causing such manifestations.
- If the lower thoracic region is damaged, the pain is concentrated in the abdominal cavity and simulates intestinal pathologies, but there is no relationship with the quality of food and diet. The intensity of pain increases mainly due to physical activity.
- Disorders of the reproductive or urinary system also develop as a result of distortion of the innervation of organs.
- Damage to the upper segment of the thoracic region causes the appearance of symptoms such as pain in the esophagus and pharynx and the sensation of a foreign body in the pharyngeal cavity or in the retrosternal region.
Atypical symptoms are characterized by their manifestation in the late afternoon, absence in the morning and appearance when provoking factors appear.
Dorsago and dorsalgia
Signs of thoracic osteochondrosis include two vertebral syndromes:
- back;
- dorsalgia.
Dorsago is a sudden, sharp pain that occurs in the thoracic region, mainly when standing up after a long period of sitting in an inclined position. The intensity of the pain may be so great that the person has difficulty breathing. In this case, there is significant muscle tension and limited range of motion in two sections: the cervicothoracic and thoracolumbar.
Back pain is characterized by a gradual and imperceptible development. The intensity of the pain is mild; Sometimes you can talk more about a feeling of discomfort than a pain syndrome. Main features:
- the duration can be up to 14 to 20 days;
- an intensification of the syndrome is observed when leaning to the sides, forward or when breathing deeply;
- with upper back pain, movements in the cervicothoracic region are limited, with lower back pain, movements in the lumbar-thoracic region are limited;
- the pain intensifies at night and may disappear completely when walking;
- The increase in pain is caused by deep breathing and prolonged stay in one position.
Diagnosis
To confirm the diagnosis, the following is done:
- Bone scan. With its help you will be able to detect:
- changes in the anatomy of the damaged segment;
- disc thickening;
- vertebral deformation and displacement;
- difference in the height of the intervertebral discs.
- Computed tomography (CT) and magnetic resonance imaging (MRI) are more accurate methods because they provide a layer-by-layer image of the affected area.
- Electromyography is performed to differentiate neurological symptoms that develop as a result of compression of nerve roots in thoracic type of osteochondrosis. An examination is prescribed if the following signs occur:
- impaired coordination of movements;
- headache;
- dizziness;
- pressure fluctuations.
- Laboratory tests: performed to determine the level of calcium in the blood and ESR (erythrocyte sedimentation rate).



























